I can’t even count the amount of times patients have walked in demanding antibiotics for their cold or flu. They have a cough, runny nose, fevers and they want antibiotics for their infection. So why don’t you get them? The answer is bigger than you think.
There are different types of infections; the main types are bacterial, viral and parasitic. A bacterial infection includes diseases like cellulitis (skin infection), pneumonia, tonsillitis and strep throat. A viral infection includes diseases like the flu, hepatitis, HIV, EBV (also known as ‘mono’ or ‘glandular fever’). A parasitic infection includes diseases like ring worm, giardia and toxoplasmosis. We have different drugs to treat each different type of infection.
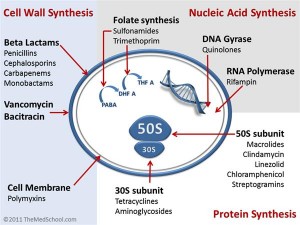
How do antibiotics work? Antibiotics attack bacteria by acting on a specific process that allows the bacteria to survive or reproduce. There are 7 main classes: macrolides, aminoglycosides, tetracyclines, beta-lactams, sulfonamides, glycopeptides and quinolones. Each different class of antibiotics acts on a different part of the bacteria to either destroy it (bacteriocidal) or stop it reproducing (bacteriostatic). For example, some classes of antibiotics inhibit DNA synthesis of the bacteria, while others damage the cell wall of the bacteria. Antibiotics have been designed to specifically target different processes or parts of the bacteria.
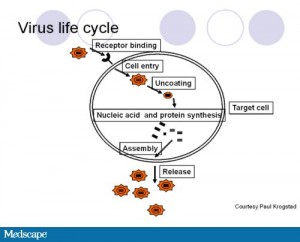
What’s different about viruses? Viruses are different to bacteria because in order to function they invade and take over our own cells (the target cells) and then use these cells as factories to replicate. It is a harder system to target. Anti -virals do exist for disease like HIV and hepatitis but it is difficult to design anti-viral medication because the anti-virals need to differentiate the virus from our own cells. This is why antibiotics will not work for viral infections like the flu.
Can’t my doctor just give them to me anyway, just in case? This type of prescribing happens more often than it should. There is a good reason doctors try not to prescribe antibiotics when they are not required. One reason is the side effects and risks to the patient for a medication that will not work. Another reason is antibiotic resistance. When we overuse antibiotics, the bacteria evolve and develop new ways to fight off our antibiotics. For example, they may evolve tougher cell walls, or a pump on their surface to pump out the toxic antibiotics. This has resulted in some bacterial infections becoming ‘resistant’ to certain classes of antibiotics. And the worrying thing is, our design and development of new antibiotics is not keeping up with bacterial evolution. This is bad.
Your doctor may not always mention it, but if you are given antibiotics it is very important that you complete the course, even if you feel better. It is also important not to take leftover antibiotics (either yours or someone else’s) because this will lead to an incomplete course of treatment. Why is this important? If you do not finish a full course of antibiotics, you may start to feel better, but you haven’t completely killed off all of the bacteria in your body. This means that the left over bacteria can ‘learn’ how to evade the antibiotics and evolve and become resistant. You then spread these bacteria through your day to day activities.
We all have a responsibility to prevent bacterial resistance. If you have a cold or a flu, don’t pester your doctor for antibiotics. Not only will they not help, they can cause harm to the human race if used inappropriately!

